Rock Steady Boxing is now offered at the Paul H. Broyhill Wellness Center. This is a fitness program designed for people with Parkinson’s Disease. Read More: Rock Steady Boxing designed for people with Parkinson’s


Rock Steady Boxing is now offered at the Paul H. Broyhill Wellness Center. This is a fitness program designed for people with Parkinson’s Disease. Read More: Rock Steady Boxing designed for people with Parkinson’s

The Rehabilitation Center offers a Therapy Pool for Rehab patients. Our therapists are trained to help you with our state-of-the art pool equipment. Read More: Therapy Pool
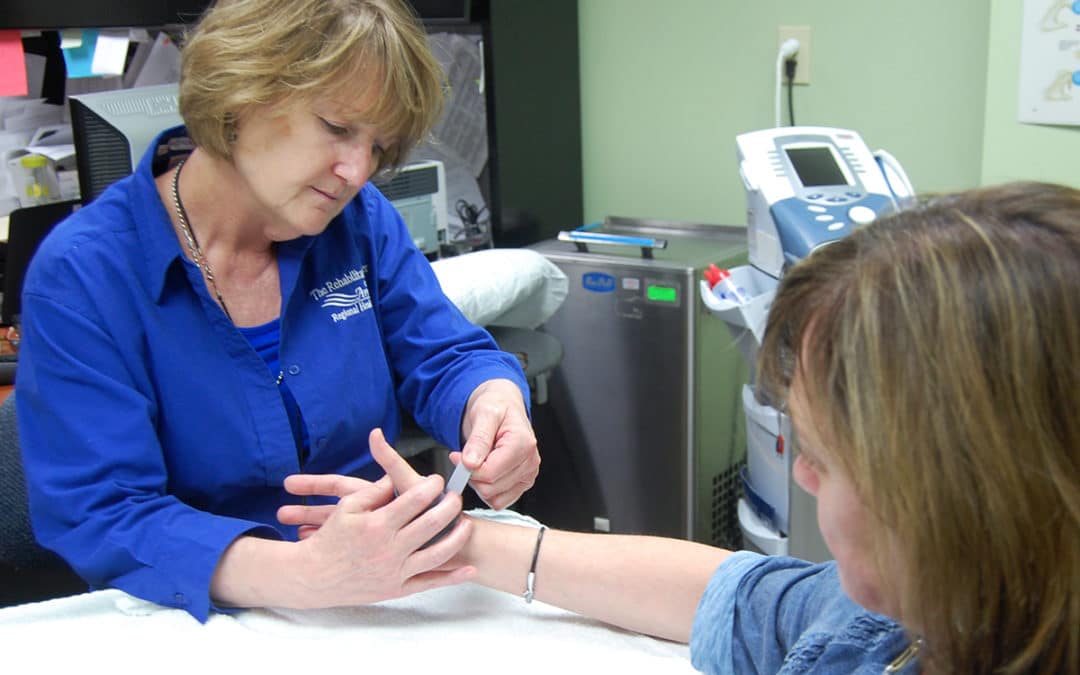
Occupational therapy is a science-driven healthcare profession that examines the person, the environment, and the tasks the person desires to perform. The goal is to restore the person’s function or adapt the task or environment for optimal performance. Read More: What is Occupational Therapy?

Although sitting on the comfy couch in your pajamas might sound like a more comfortable way to work, you are at risk for musculoskeletal strain or pain from awkward sitting postures. Here are some tips for setting up a home office and preventing pain and injuries. Read More: 4 steps to a pain-free home office

A balance disorder is a condition that makes you feel unsteady as if you are moving or spinning even though you are standing still or lying down. Studies indicate that “dizziness” is among the three most common complaints encountered in the primary care setting. Read More: Balance Disorders: Common Causes and Treatments

Dry needling doesn’t sound like a fun day at the park but intramuscular stimulation, as it is sometimes called, is a treatment used to target and restore muscle function while reducing muscle pain. Read More: Dry needling therapy to increase muscle function and reduce pain

The Rehabilitation Center is dedicated to practicing Physical and Occupational Therapy within an evidence-based, clinical practice paradigm. Read More: All Physical Therapy and Rehabilitation Services

Our therapists provide customized, therapeutic interventions to meet a wide array of individual needs. Read More: Physical and Occupational Therapists